Gloves - Keeping You and Your Patient Safe: Top 5 Glove Mistakes You May Not Know You're Making

It's easy for us to open the box of gloves, put them on, do our job, and take them off without giving them a second thought. But when we think about it, are we making infection control mistakes with the gloves we use many times during the day? We must consider glove choice based on the rationale for using a particular glove. Medical gloves are one component of our standard personal protective equipment (PPE) used in our daily clinical sessions. PPE protects the wearer and the patient from infection or illness during treatment procedures or examinations. All medical gloves are considered one-time-use disposable items regulated by the Food and Drug Administration (FDA) and Health Canada. They are considered a Class 1 medical device in the USA, and in Canada, they fall under a class 2 medical device. The FDA (US) and Health Canada (Canada) both review and regulate these devices to confirm that they meet leak resistance, tear resistance, and biocompatibility criteria.1,2 We as health care providers wear medical gloves for the following principal reasons:
- To reduce the risk of contamination of our hands with blood or other body fluids
- To reduce the risk of spreading pathogens to the clinical environment
- To reduce the transmission of pathogens from the patient to healthcare worker, from healthcare worker to patient, and from patient to patient.3
Gloves alone do not provide complete protection against hand contamination
Clinical research confirms that gloves effectively prevent significant contamination of healthcare workers' hands. Gloves are also a substantial barrier to transmitting pathogens in clinical settings. However, we must be aware that gloves do not provide complete protection from hand contamination. Pathogen transmission can occur through glove defects such as tears and manufacturing defects. Improper removal of gloves following dental procedures by user error can contaminate the wearer. We must consider that proper hand hygiene with the right hand sanitizing procedure and hand hygiene products remain the essential assurance that hand decontamination is complete following treatment and glove removal.3
5 Glove Mistakes You Might Not Know You Are Making
1. Choosing the Wrong Glove For the Job
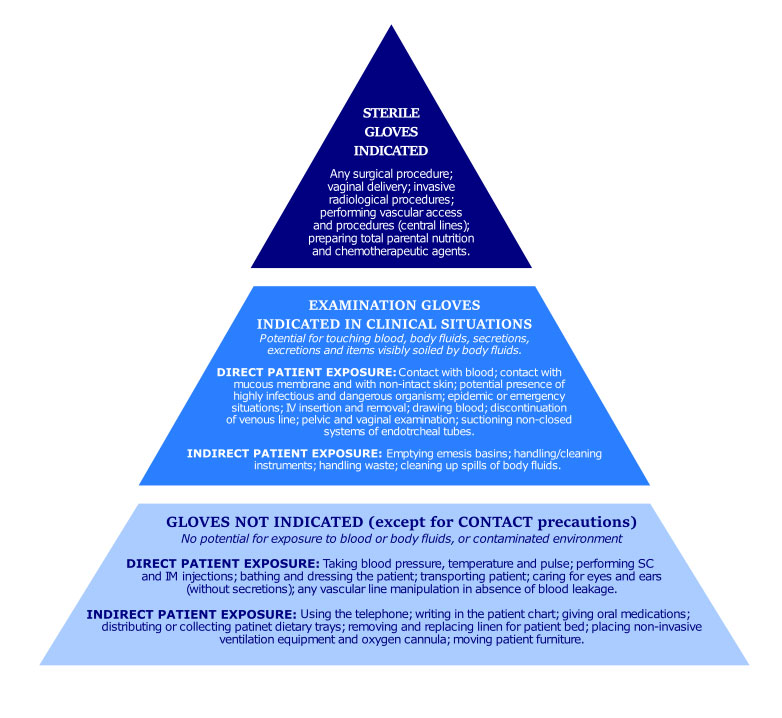
Healthcare workers must choose the right glove for the situation in a medical or dental setting. We must wear the appropriate glove based on standard and contact precautions. The inappropriate use of gloves results in a waste of resources and may increase the risk of pathogenic organism transmission. We should plan and perform procedures in a rational sequence to use non-touch techniques that minimize the need for frequent glove changes during the same procedure. For example, having all supplies necessary for the procedure accessible without needing to open drawers or cabinets eliminates the need to remove and put on new gloves. The gloves' selection should be based on the type of setting, the task to be performed, the likelihood of exposure to bodily fluids, the length of use, the amount of stress on the glove, and the glove material that needs to be considered before selecting the appropriate glove. The glove pyramid graphic below 3 identifies some examples of all healthcare clinical procedures and the gloves recommended or necessary. You should, however, perform proper hand hygiene procedures regardless of the suggestion for glove use. 3
The 4 Types of gloves Commonly Used in Dental Settings:
- Sterile
- Indicated for performing any invasive sterile procedure, including but not limited to dental surgical procedures (e.g., periodontal, oral surgery). Includes sterile surgical gloves
- Non-sterile
- Indicated in situations when there is potential for contact with infectious material (e.g., blood, other body fluids, microorganisms). Includes nitrile, latex, medical vinyl.
- Non-Medical
- Used for some housekeeping procedures (e.g., disinfection and cleaning). Includes vinyl gloves. .
- Utility
- Used for manual cleaning of instruments and decontamination with harsh chemicals (e.g., central sterilization instrument reprocessing area and cleaning of environmental surfaces). Includes gloves like our instrument processing utility gloves.
2. Substituting Glove Use for Hand Hygiene
Putting on a pair of examination gloves without proper hand hygiene does not adequately protect the healthcare worker or patient. Hand hygiene is not a step to be missed. Hand hygiene is a general term that applies to routine hand washing with soap and water, cleaning hands with an antiseptic alcohol-based hand rub, and surgical antisepsis. To follow infection control procedures in the dental office, removing all jewelry and keeping nails trimmed and neatly filed should proceed with handwashing. The Centers for Disease Control and Prevention (CDC) and Health Canada recommend that hand hygiene be performed:
- Before and after treating patients
- Before leaving the dental operator
- After touching objects contaminated by blood, secretions, or saliva
- When hands are visibly soiled
- After removing gloves that are torn, cut, or punctured
- And before replacing gloves
3. Using Non-Approved Hand Lotions
Always consider the ingredient in hand lotions before donning exam gloves. Hand lotions or creams must be water-based and petroleum-free, as petroleum-based products can weaken glove material. Using products such as Renovo Hand Moisturizer will ensure that the glove material will not degrade. Most gloves are powder-free; however, alcohol-based hand rubs can interact with the powder in powdered gloves. Glove liners can be worn under examination gloves to keep hands warm and dry without compromising the integrity of the glove.
4. Improperly Fitting and Incorrectly Donning Gloves

Gloves must fit correctly and are comfortable to wear during all patient treatment. The recommendation from the CDC and Health Canada is examination gloves must be put on only after proper hand hygiene, and gloves must extend to cover the wrist of the isolation gown. Gloving must occur before a sterile procedure when anticipating contact with blood or body fluid, including non-intact skin and mucous membranes. The World Health Organization provides and recommends the following donning instructions.
- Perform hand hygiene
- Take out a glove from the original box
- Touch only a restricted surface of the glove corresponding to the wrist (at the top edge of the cuff)
- Don the first glove
- Take the second glove with the bare hand and touch only a restricted surface of glove corresponding to the wrist
- To avoid touching the skin of the forearm with the gloved hand, turn the external surface of the glove to be donned on the folded fingers of the gloved hand, thus permitting to glove the second hand
- Once gloved, hands should not touch anything else that is not defined by indications and conditions for glove use
Note: Gloves with Rapid-Don technology allow for easier donning when hands are damp.
5. Improper Removal of Gloves

The correct technique for removing or doffing gloves prevents healthcare workers from contaminating their hands and resulting in pathogen transmission.
Remove all gloves:
- After patient treatment
- Immediately if gloves are damaged, or non-integrity is expected
- When there is an indication for hand hygiene
Don new gloves for surface cleaning and disinfection. Never reuse or reprocess gloves. Both Health Canada and the CDC provide and recommend the following doffing instructions:
- Using a gloved hand, grasp the palm area of the other gloved hand and peel off the first glove
- Hold removed glove in gloved hand
- Slide fingers of ungloved hand under the remaining glove at wrist and peel off second glove over first glove
- Discard gloves in a waste container
- Perform hand hygiene
Gloves are essential to our providing a barrier to disease-causing pathogens. And glove quality and integrity have improved over the years. We must continue to correctly choose and wear our equipment to ensure our health safety and prevent disease transmission to our colleagues and patient.
Sources:
- U.S. Food and Drug Administration. (2020, March 20) Medical Gloves. https://www.fda.gov/medical-devices/personal-protective-equipment-infection-control/medical-gloves
- Health Canada (2016, April 04) Medical Gloves. https://www.canada.ca/en/health-canada/services/drugs-health-products/medical-devices/activities/announcements/notice-medical-gloves.html
- World Health Organization. (n.d.) Glove Use Information Leaflet. https://cdn.who.int/media/docs/default-source/integrated-health-services-(ihs)/infection-prevention-and-control/hand-hygiene/tools/glove-use-information-leaflet.pdf?sfvrsn=13670aa_10
- Centers for Disease Control and Prevention. (n.d.) Sequence for Putting On Personal Protective Equipment. https://www.cdc.gov/hai/pdfs/ppe/ppe-sequence.pdf
- Centers for Disease Control and Prevention. (n.d.) How to Safely Remove Personal Protective Equipment.https://www.cdc.gov/hai/pdfs/ppe/ppe-sequence.pdf
- Public Health Ontario (Accessed 2022, June 17th) Recommended Steps: Putting On Personal Protective Equipment (PPE): https://www.publichealthontario.ca/-/media/documents/ncov/ipac/ppe-recommended-steps