'Mask' Confusion: From Uncertainty to Understanding

Face masks have become a common sight for the human population, especially since the Covid-19 global pandemic hit in 2020. At the beginning of the pandemic, public health agencies were hesitant to recommend the consistent use of face masks. The general public was also uncertain of what to believe. To mask or not to mask, this was the question. However, after the World Health Organization acknowledged that the virus could be airborne and linger in the air for hours, masking as a weapon against the coronavirus became a preventive measure to keep virus transmission in check. It was not unusual to see face masks hanging from every car rearview mirror, offered at the entrance to every business, or mandated at every work environment. Face coverings became a fashion statement when people made cloth face coverings in many styles and fabrics. This cloth covering was acceptable for the general public and is considered a form of universal source control.
Within the healthcare system, masking has been commonplace for over a century. Our decision to increase the consistent and habitual use of masking increased as the pandemic spread worldwide. Over the past year or so, the CDC has updated the strict guidelines for healthcare facilities. As of May 5, 2023, the Government of Canada ended the COVID-19-related public health emergency after the World Health Organization (WHO) held a meeting of its International Health Regulations (IHR) Emergency Committee. The Centers for Disease Control and Prevention no longer recommends routine universal masking in health care settings. Many clinicians and staff in hospitals, clinics, and nursing homes have stopped wearing masks. This is unfortunate as patients pay the price for the objection to masking by healthcare personnel. The Government of Canada continued ongoing monitoring, with contribution and assessment of the global epidemiology of COVID-19. However, it was still recommended that personal protective practices, such as well-fitting masks remained in place to reduce risk and limite the burdern on the healthcare system.
Masking in Dentistry
The practice of using facemasks in dentistry dates back to the early 1900s. Early forms of the face mask were constructed from layers of cotton gauze. Over the last century, face mask form, function, and material have developed. Today, surgical masks protect patients from the wearers' respiratory emissions. Within the United States, surgical masks are cleared for marketing by the U.S. Food and Drug Administration (FDA). They can be labeled as surgical, laser, isolation, dental, or medical procedure masks. Not only are they regulated and cleared by the FDA, but the Occupational Safety and Health Administration (OSHA) recommends surgical masks to protect the wearer from direct exposure to splashes and sprays of infectious body fluids and blood.
Most dental procedures produce aerosol from handpieces, ultrasonic scalers, and air/water syringes. The size of the droplet and airborne particle determines the level of mask filtration needed to protect us. Aerosolized bacteria and virus particles smaller than 50 microns in diameter are known as aerosols. Those smaller aerosolized particles of .5-10 microns remain afloat in the air for prolonged periods and can penetrate and lodge in the smaller passages of the lungs, causing infection.
The dental profession has been one of the most compliant in wearing and accepting PPE (Personal Protective Equipment). A study in the Journal of Global Oral Health found that over 75% of the study participants agreed that routine mask usage among dentists makes dentists better protected compared to other healthcare providers, and over 92% believed it was easier for the dentist to adapt to the behavioral changes needed during the pandemic due to the customary occupational use. However, over 83% believed that there is still a lack of awareness among dentists regarding the proper selection, usage, and disposal of masks. This reflects consistent but improper mask practices among dentists. The study also highlights the need to increase awareness regarding the selection and correct usage of disposable masks to minimize disease transmission in healthcare settings.
Testing, Regulating, and Marketing Masks
We know masks are integral to our PPE (Personal Protective Equipment) protocol, but how do we choose what mask to wear? To help us clarify what mask to use for dental procedures, agencies such as NIOSH (National Institute for Occupational Safety and Health) and ASTM (American Society for Testing and Materials) have provided testing criteria to evaluate a mask's effectiveness.
Summary of standard tests for evaluating mask effectiveness.
|
Test |
Details |
Organization/Regulation |
|
Particle filtration efficiency |
·Uses charge-neutralized NaCl aerosols at a high, fixed flowrate ·Masks/respirators are preconditioned 24 hours before testing. ·Evaluates filtration efficiency. ·Highly conservative and stringent test. |
NIOSH |
|
Bacterial/Viral filtration efficiency |
·Uses various bacteria/viruses suspended in aerosols. ·Evaluates filtration efficiency. ·To receive a medical/surgical grade mask rating, a minimum of 95% filtration is required. ·Moderate or high protection masks must have a 98% or greater bacterial filtration rate.
|
FDA |
|
Fluid resistance |
·Uses synthetic blood squirted at the mask at various pressures. (80,120, or 160 mmHg to qualify for low, medium, or high fluid resistance. ·Mask is qualitatively evaluated to determine if blood has penetrated. |
ASTM (test method F1862) FDA (surgical masks)
|
|
Pressure differential (ΔP) |
·Determines the "breathability" of a mask ·Measures difference in pressure up and downstream of mask ·High ΔP means the mask is difficult to breathe in, but better filtration |
|
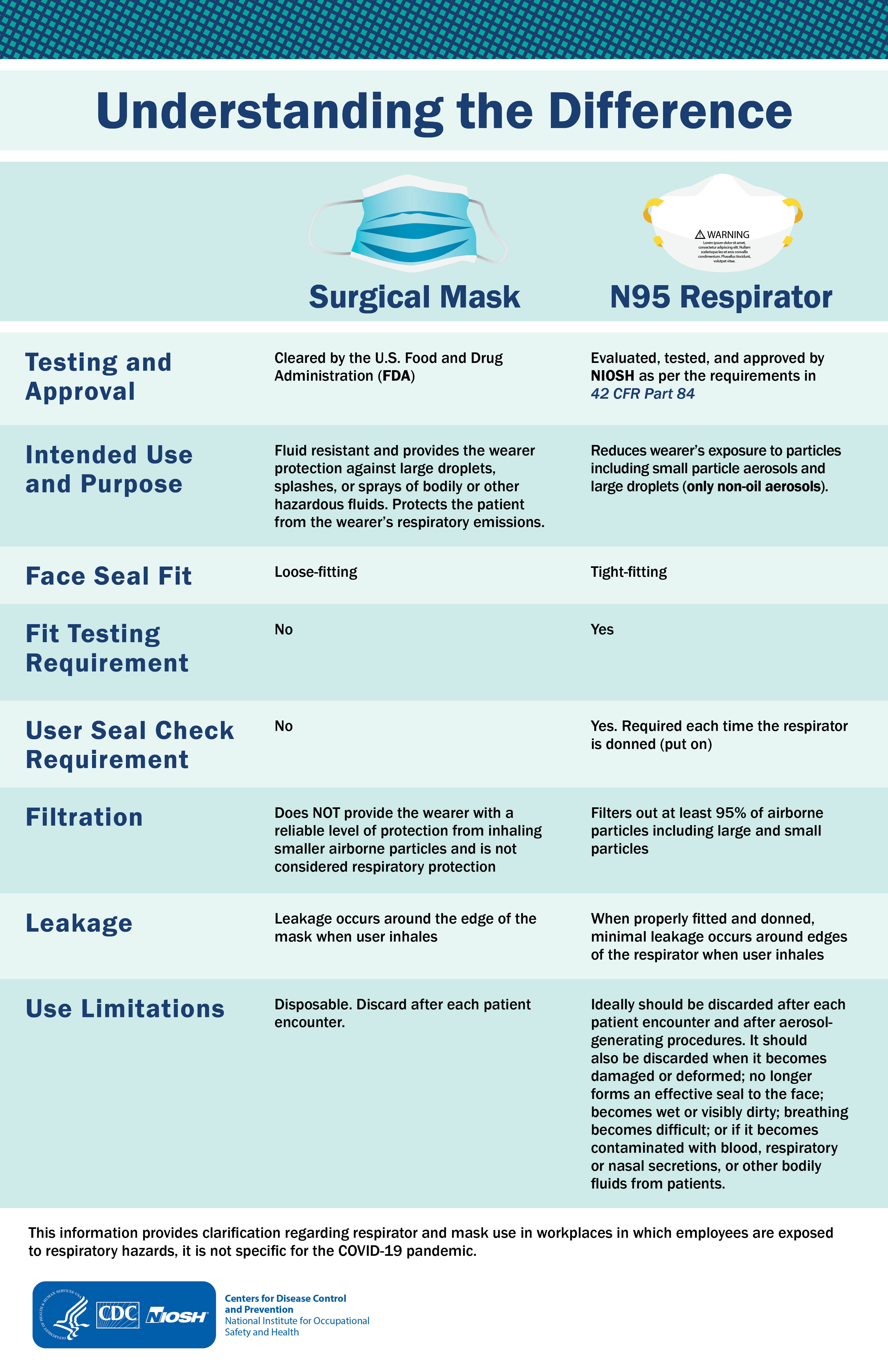

Image Source: https://www.cdc.gov/niosh/npptl/images/infographics/UnderstandingInfoGraphLG.jpg
ASTM Performance Metrics and Levels
|
Test |
ASTM Level 1 |
||
|
Fluid Resistance |
80 mmHg |
120 mmHg |
160 mmHg |
|
Filtration - BFE |
≥ 95% |
≥ 98% |
≥ 98% |
|
Filtration - PFE |
≥ 95% @ 0.1 μg |
≥ 98% @ 0.1 μg |
≥ 98% @ 0.1 μg |
|
Delta P –Breathability |
< 4.0 mm H2O/cm3 |
< 5.0 mm H2O/cm3 |
< 5.0 mm H2O/cm3 |
A Word About Respirators
Respirators differ from surgical and procedure masks as they are designed to reduce the risk of the wearer inhaling chemicals, dust, gas, vapors, or infectious agents. They are used in many industries, including healthcare. Respirators may cover the entire head, such as a Powered Air-Purifying Respirator (PAPR) or one that covers the nose and mouth. NIOSH regulates and certifies respirators then they are cleared for sale in the U.S. by the FDA. Before wearing them, the wearer must follow the guidelines set forth by OSHA.
OSHA standards require:
-
- Respiratory health questionnaire and screening
- Fit testing for the specific respirator to be used
- Annual training for the use of respirators
- Training for maintenance and care of respirators
Respirators are rated by the percentage of airborne particles filtered in testing when using the most penetrating particle size. A respirator that filters 95% is given a rating of 95, one that filters at least 99% of the particles is given a 99, and those that filter 99.7% are given a rating of 100.
Image Source: https://www.cdc.gov/niosh/npptl/images/infographics/FY17N95infographicWhatAre.jpg
Compliance and Instruction for Use
This testing and regulation ensure that the appropriate level mask will protect the wearer from exposure to spray, splatter, or aerosols during the procedure. Surgical masks are a protective barrier against liquid spray and splatter, offering moderate filtration effectiveness against pathogenic particles. If higher filtration is needed, especially during aerosol-generating procedures, respirators such as N95 masks will be a better option. Understanding the specific design features of masks and respirators is only a part of the ability of the mask to keep us safe from disease transmission. As with many things, wearing a proper mask, complying with the instructions, and adhering to instructions for use are essential for effective protection. Follow these steps to ensure you are using the masks correctly:
Before Putting on the Mask
-
- Wash your hands for at least 20 seconds with soap and water or use alcohol-based hand sanitizer.
- Inspect the mask: check for any damage or defects in the mask.
Putting on the Mask
-
- Hold the Mask: Hold the mask through the ear loops with the colored side facing outwards.
- Secure the mask: Place the mask over your nose and mouth, ensuring it covers both areas.
- Metal strip: If present, pinch the metal strip at the top of the mask to fit it around your nose.
- Layers: Remember that surgical masks have three layers:
-
- Outer layer: repels water, blood, and other body fluids.
- Middle layer: filters specific pathogens.
- Inner layer: absorbs moisture from sweat and exhaled air.
-
-
During Use
-
- Avoid touching the mask: refrain from touching the mask while wearing it.
- Proper fit: ensure the mask fits snugly over your nose, mouth, and chin.
- Make sure there are no gaps on the sides of the mask.
Taking off the Mask
-
- Remove gloves before removing the mask.
- Avoid contamination: hold the mask by the loops, ties, or bands only (not the front of the mask).
- Remove carefully: unhook both earloops or untie the strings.
- Dispose: dispose of the mask after each patient or if the mask becomes wet during treatment.
- Wash hands: Wash your hands thoroughly or use hand sanitizer.
Final thoughts
The navigation of mask-wearing in a dental practice demands our attention to detail. We must understand the importance of these simple tools in protecting both ourselves and our patients. From the early days of using cotton gauze to todays surgical masks and respirators, we've seen significant progress.
Even as the global health crisis has eased and guidelines have changed, we must remember the vital role masks play in controlling infections, especially in dentistry where aerosols are common. By embracing advancements in mask technology and following strict testing standards, we ensure we choose the right masks and use them correctly.
Each step in the process matters, from checking masks before putting them on to carefully removing them afterward. These actions aren't just about safety; they're about caring for our patients and community. Let's continue to prioritize proper mask use, knowing that it's essential for everyone's well-being.
References
1. Ameena NB, Ramanarayanan S, Kuruvilla S, Latti P. Perceptions and usage of masks among dental professionals – The impact of COVID. J Global Oral Health 2022;5:75-9.
2. Ju, T. J., Boisvert, L. N., & Zuo, Y. Y. (2021). Face masks against COVID-19: Standards, efficacy, testing and decontamination methods. Advances in Colloid and Interface Science, 292, 102435. https://doi.org/10.1016/j.cis.2021.102435
3. Public Health Agency of Canada. (2023, May 5). Update on the COVID-19 situation in Canada-May 5, 2023. https://www.canada.ca/en/public-health/news/2023/05/update-on-the-covid-19-situation-in-canada--may-5-2023.html