Do You Have a Caries Risk Program In Your Office?

As dental professionals, it is not new news that enamel falls prey to constant demineralization. In the Enamel 101 of dentistry, we learned the fact that hydroxyapatite can be attacked by acids and break down if there is not a remineralization balance. The ideal balance is to stop acid attacks period.
However, like every dental office lunchroom filled with chocolate and various baked goods, our clients are human and like a sweet treat occasionally. In some of our client populations, the etiology of the demineralization is linked to systemic impacts revolving around xerostomia from medication, underlying health issues, and/or cancer treatments. Our first duty is to screen to see where the client falls on the teeter-totter of demineralization and remineralization.
What is a Caries Risk Assessment?
The basic rationale is to evaluate the environmental and biological contributing factors balanced with protective factors to see what is causing demineralization and what is causing remineralization. A caries risk assessment is:
- analyzing the balance between demineralization and remineralization,
- concluding a proper risk level of low, moderate, or high, and
- gearing the remineralization solutions based on that risk level.
Our second job is to
- determine the protective factors needed for the client or identify the ones the client is already implementing, consciously or unconsciously.
A Method To Solve The Problem
In our first duty of screening, dental professionals are not out to dodge a proper caries risk assessment. Contrary, we are all trying to determine an effective and efficient method to employ to complete the task.
Well, a solution is here!!! A solution that I can 100% vouch it works because I have been using it in my dental hygiene practice for the last 6 years.
We have all heard of the CAMBRA (Caries Management By Risk Assessment) approach, it consists of evidence-based screening forms divided into the age groups of 0-5 and 6 and over.
The question becomes do you have to use these lengthy forms, or can you use the theory of CAMBRA to compile and implement a shorter, yet ethically effective approach?
Well, another solution is here. How about a neatly organized table that encompasses the evidence from CAMBRA and allows the dental professional to complete the screening chairside with full client interaction and participation? Voila, see below the table I personally use in my practice.
I have incorporated the table on the back of my main medical history form forcing me to re-visit the caries risk assessment every time a full medical history form is required.
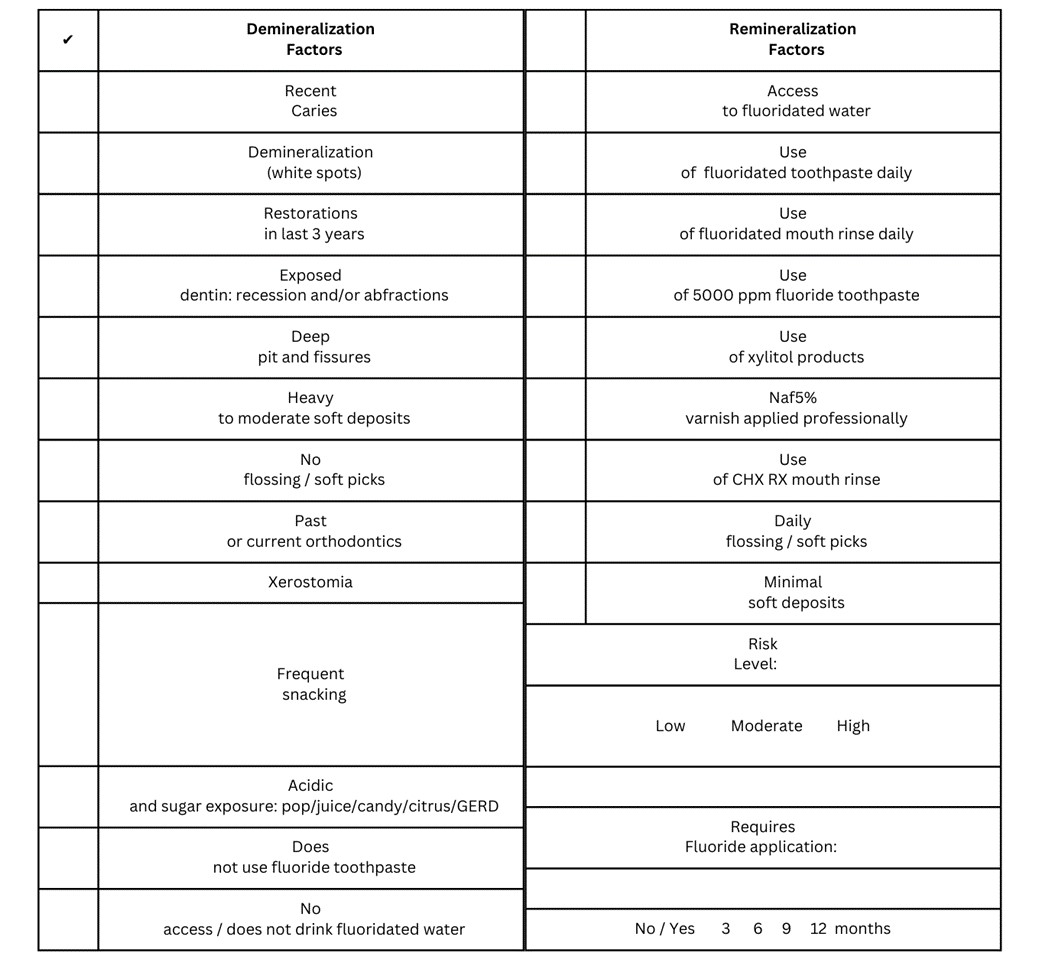
(Table courtesy of Positive Impact Dental Coaching)
This table is the solution to the demineralization and remineralization teeter-totter, leaving out any guesswork and framing contributing factors to both risk and protection. The protection at a professional level is simple, we all have it in our offices, naf5%, fluoride varnish. In some geographical areas, the decision makers for the structure and categories of the dental fee guide have divided the professional fluoride applications based on the type of fluoride used.
For example, in Ontario the ODA has established a fluoride varnish code for billing. Fluoride varnish is not a newcomer in the product lineup of dentistry. Every dental office’s caries risk management program MUST include fluoride varnish. There are countless studies proving the efficacy of naf5% whether applied in private dental clinics or mass application with public health prevention programs.
How will the dental professional decide who needs fluoride varnish and when?
The fantastic caries risk assessment table graciously provided above that not only gathers the ‘demin and remin’ data but assigns the risk level and a regimen for fluoride varnish application. This solution meets 'process-of-care' in an evidence-based decision-making approach as well as record keeping showing how you as a dental professional concluded that someone in your practice needs or does not need fluoride varnish.
Note, in the table provided many clients regardless of age fall into some risk level of needing fluoride varnish. It is a complete myth that only children need a fluoride varnish application. Insurance dependencies aside, when a client is well educated on the ‘demin and remin’ teeter-totter, they will choose to receive fluoride varnish.
Going Forward
As of this exact moment, you have a caries risk assessment system and are well on your way to building a practice that supports the service of fluoride varnish from a risk management platform. maxill is a leader in cost-effective quality fluoride varnish, offering a tasty variety of naf5% in mint, bubble gum, and caramel.
This is not only a solution for proper client care but a practice builder for the office’s financial health. We all know a dental office has a business management aspect and a well-structured caries risk assessment program delivers both quality client care and ethical business support as the overall cost of maxill’s fluoride varnish allows for a solid return. Need assistance with implementation, do not hesitate to reach out. I would be thrilled to share my success story of the ‘demin and remin’ teeter-totter!